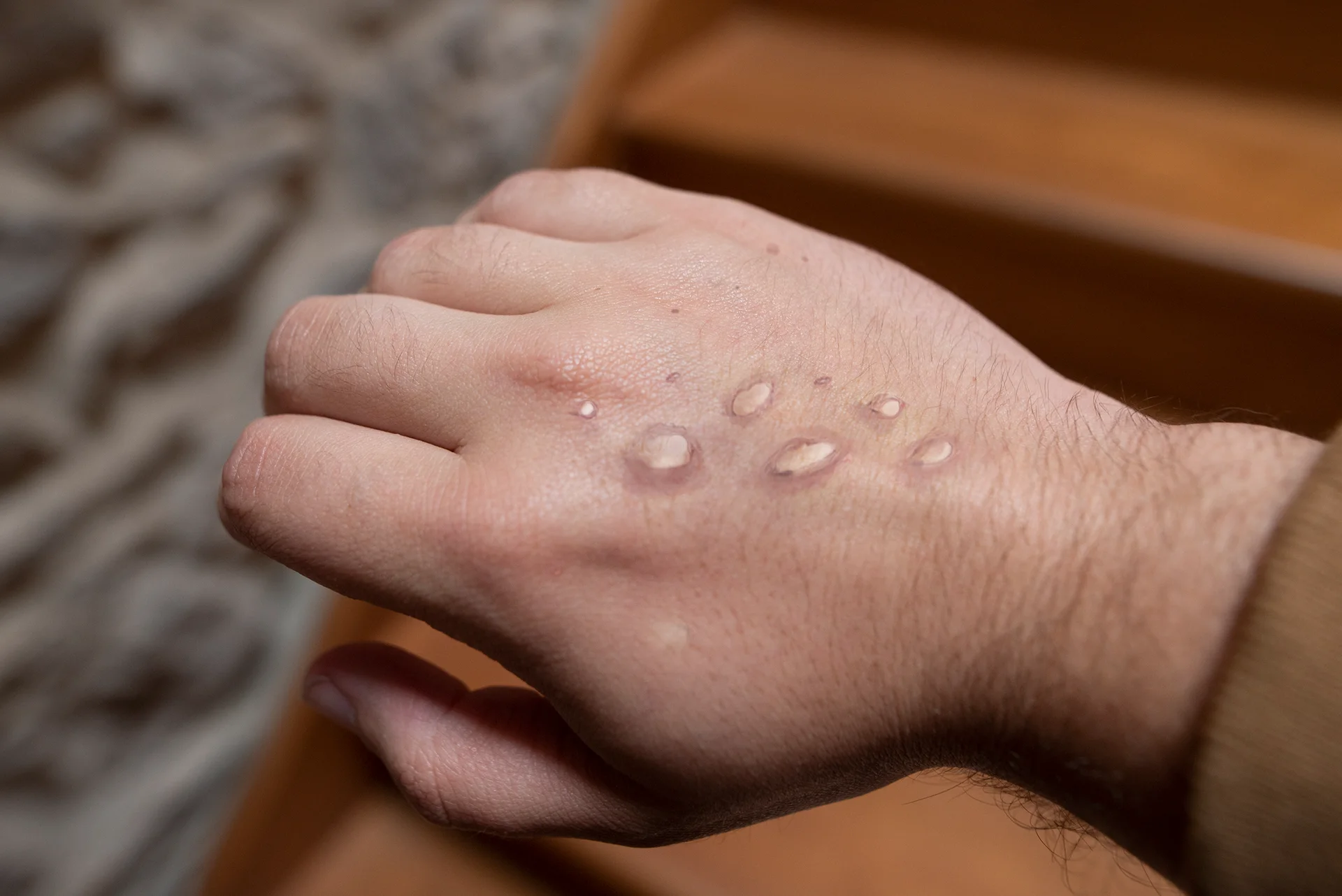
Smallpox is a highly infectious and deadly disease caused by the variola virus. It has plagued humanity for centuries and was responsible for millions of deaths before being eradicated in 1980 through a global vaccination campaign.
Natural immunity to smallpox is acquired through exposure to the virus, either through infection or vaccination. The immune system produces antibodies that recognize and neutralize the virus, providing protection against future infections. In this article, we will explore the intricacies of natural immunity to smallpox and its implications for public health.
Impact of Smallpox on Human History
Smallpox is one of the deadliest diseases in human history, responsible for an estimated 300 to 500 million deaths in the 20th century alone. It has been around for thousands of years and has affected almost every part of the world. The disease is highly contagious and spreads through respiratory droplets or contact with contaminated objects.
Smallpox outbreaks have had a significant impact on human history. It has ravaged populations, leading to social upheaval, economic collapse, and political instability. In some cases, it has wiped out entire communities and civilizations. For example, smallpox was one of the main factors that contributed to the decline of indigenous populations in the Americas after European colonization.
Smallpox eradication and the role of vaccination
Despite its devastating impact, smallpox also played a role in shaping modern medicine. The first vaccine was developed by Edward Jenner in the late 18th century using cowpox virus, which provided protection against smallpox. This discovery paved the way for vaccination programs that would eventually lead to the eradication of smallpox.
The eradication of smallpox remains one of humanity’s greatest achievements in public health. It required a coordinated global effort involving governments, organizations such as WHO (World Health Organization), and thousands of healthcare workers. The last known natural case occurred in Somalia in 1977, and after a rigorous vaccination campaign worldwide led by WHO between 1967-1980, smallpox was declared eradicated from the world population by WHO on May 8th 1980 – marking an extraordinary milestone in medical science history.
Definition of Natural Immunity
Natural immunity refers to the immune system’s ability to recognize and defend against pathogens without prior exposure to them through vaccination or infection.
Also known as innate immunity, is the first line of defense against pathogens that the body encounters. It is a nonspecific defense mechanism that provides immediate protection against a wide range of pathogens, including bacteria, viruses, fungi, and parasites. Unlike adaptive immunity, which requires prior exposure to antigens through vaccination or infection, natural immunity is present at birth and does not require prior exposure to pathogens.
Natural Immunity Components
The natural immune system consists of physical, chemical, and cellular barriers that prevent pathogens from entering the body, such as the skin, mucous membranes, and stomach acid. It also includes innate immune cells, such as macrophages, natural killer cells, and dendritic cells, which recognize and respond to pathogens based on common molecular patterns found on many pathogens.
When a pathogen breaches these barriers and enters the body, the innate immune system responds rapidly to contain and eliminate the pathogen. Innate immune cells engulf and destroy the pathogen, while also releasing cytokines that recruit other immune cells to the site of infection and activate the adaptive immune response.
Factors contributing to natural immunity against smallpox
There are several factors that contribute to natural immunity against smallpox, including genetic factors and previous exposure to similar viruses.
Genetic factors play a significant role in determining an individual’s susceptibility to infections such as smallpox. Studies have shown that certain genes associated with the immune system may confer greater protection against smallpox, while others may increase susceptibility.
Previous exposure to similar viruses, such as cowpox, can also provide cross-protection against smallpox. Cowpox is a less virulent virus that is closely related to smallpox and was used in the first vaccine developed by Edward Jenner in 1796. Individuals who were vaccinated with cowpox were found to be protected against smallpox, indicating that the two viruses share some degree of antigenic similarity.
Natural immunity can also be influenced by age, sex, nutritional status, and other environmental factors. While natural immunity provides some degree of protection against smallpox, it is not foolproof and can vary widely between individuals depending on their unique circumstances. Vaccination remains the most effective method for preventing the spread of smallpox and protecting individuals at risk of infection.
Vaccination as a method of acquiring immunity
Vaccination is a highly effective method of acquiring immunity to smallpox. Here we will discuss the history of smallpox vaccination and the role of vaccinia virus in smallpox vaccines.
Smallpox vaccination has been around for over 200 years, starting with Edward Jenner’s discovery of cowpox vaccination in 1796. The first vaccine involved taking material from a cowpox lesion and inoculating it into a person’s skin, which provided protection against smallpox. This was followed by the development of other types of vaccines, including those made from calf lymph and human lymph.
The widespread use of smallpox vaccines began with the establishment of compulsory vaccination programs in Europe in the mid-19th century. These programs were successful in reducing the incidence of smallpox, but they were also controversial due to concerns about vaccine safety and individual rights. In many countries, opposition to mandatory vaccination led to public protests and riots.
The vaccinia virus, a related but less virulent virus than variola (smallpox) virus, is used in modern smallpox vaccines. Vaccinia virus is similar enough to variola virus that it can stimulate an immune response that provides cross-protection against smallpox.
The current smallpox vaccine consists of live vaccinia virus that is grown in cell culture and then freeze-dried for storage. The vaccine is administered by scarification or puncture using a bifurcated needle that delivers the virus directly into the skin. A characteristic “take,” or pustule at the site of inoculation, develops within several days, indicating that the immune system has recognized and responded to the vaccine.
Smallpox vaccination remains an important tool for preventing outbreaks of smallpox, particularly in populations at high risk for exposure such as healthcare workers or military personnel deployed to areas where the disease may still exist. Despite its effectiveness, routine smallpox vaccination has been discontinued since 1980 because there are no known natural cases left worldwide – however stockpiles exist worldwide as precautionary measures against bioterrorism attacks involving this pathogen.
Development of Immune Response Following Vaccination
Following vaccination, the development of an immune response involves both T cells and humoral immunity. This leads to protective immunity and can provide possible lifelong protection against smallpox.
T cells and humoral immunity
T cells are an important part of the immune response following smallpox vaccination. They recognize and respond to smallpox antigens presented on infected cells, allowing for clearance of infected cells and control of viral replication. In addition, T cells can also help stimulate B cell production of antibodies which are another important component in the body’s defense mechanism.
Humoral immunity refers to the production of antibodies by B-cells in response to exposure to a pathogen or vaccine antigen. Antibodies can neutralize viruses by binding to them and preventing them from infecting host cells, as well as recruiting other components of the immune system to help clear the virus.
Protective immunity and possible lifelong protection
Protective immunity against smallpox is achieved through a combination of T cell-mediated control of viral replication and antibody-mediated neutralization of viruses before they can infect host cells. Vaccination provides long-lasting protection against smallpox, with studies showing that individuals can retain protective levels of antibodies for up to 50 years after vaccination.
It is possible that lifelong protection may be conferred by vaccination, although this has not been definitively proven due to ethical considerations regarding deliberately exposing vaccinated individuals to smallpox virus in order to test their immunity over time.
Importance of Population Immunity
Population immunity is an essential aspect of controlling infectious diseases, and herd immunity plays a crucial role in achieving this goal. Here we will discuss the concept of herd immunity, the benefits of population immunity in controlling infectious diseases, and the role of vaccination in maintaining herd immunity.
The concept of herd immunity
Herd immunity refers to the protection that occurs when a significant proportion of a population becomes immune to a particular infectious disease through either vaccination or natural infection. This provides indirect protection to those who are not immune, such as individuals who cannot be vaccinated due to medical reasons or those with weakened immune systems.
Benefits of population immunity in controlling infectious diseases
The benefits of population immunity are numerous, including reduced transmission rates of infectious diseases within communities and decreased likelihood of outbreaks occurring. This is especially important for highly contagious diseases such as smallpox, where a single case can lead to widespread transmission within a population.
Role of vaccination in maintaining herd immunity
Vaccination plays a critical role in maintaining herd immunity by increasing the proportion of immune individuals within a population. When enough people are vaccinated against an infectious disease, transmission rates decrease significantly, making it less likely that unvaccinated individuals will come into contact with an infected person and become ill themselves.
Vaccination also helps protect vulnerable populations who may not be able to receive certain vaccines due to medical reasons or age-related factors such as young children or elderly adults – this is often referred to as “cocooning” strategy which means protecting at-risk individuals by vaccinating surrounding people (family members, caretakers etc.).
Building a Strong Immune System: How SeeBeyond Medical Can Help
SeeBeyond Medical is a leading provider of health and wellness products, offering a wide range of high-quality supplements and other products through their online shop. We emphasize the importance of a healthy lifestyle and strong immune system in fighting infections.
We offer a diverse range of products that cater to different needs such as supplements for immune support, cognitive health, digestive health, weight management, and more.
Visit our shop today to discover how SeeBeyond Medical can help you improve health and build a strong immune system.